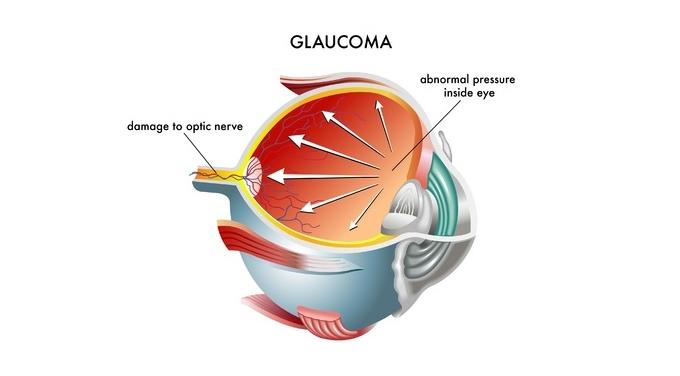
Normal Tension Glaucoma
A kind of open-angle glaucoma known as normal-tension glaucoma, also known as low tension glaucoma or normal-pressure glaucoma, damages the optic nerve without causing intraocular pressure to exceed a normal range. This is distinct from other kinds of glaucoma in which increased intraocular pressure results in optic nerve damage. Researchers still don’t fully understand the causes or mechanisms of normal tension glaucoma.
How Much Intraocular Pressure Is Normal?
It is crucial to realize that there is no such thing as safe intraocular pressure, nor is there a single value that applies to everyone. Instead, there is a normal range of pressure, and intraocular pressure might be high, normal, or below normal. The average intraocular pressure is between 15 and 16 mmHg, according to studies conducted on sizable populations in the United States, and 95% of persons have an intraocular pressure between 10 and 21 mmHg.
Regarding the distinction between primary open-angle glaucoma and normal tension glaucoma, those with P.O.A.G. do present with increased intraocular pressure levels as opposed to those with average tension glaucoma.
Who’s at Risk?
The only risk factor for the onset and progression of all kinds of glaucoma that is currently controllable is IOP. Vascular problems may contribute to LTG, albeit it is unclear why given that this patient population has a greater prevalence of migraine, Raynaud’s phenomenon, and hypotension.
LTG risk may be increased by structural variations in optic nerves with bigger disc regions. Optic disc hemorrhages are more common in LTG; if they are signs of ongoing injury, more extensive treatment may be needed. Compared to primary open-angle glaucoma, eyes with LTG more typically have focal nerve damage with paracentral field abnormalities. Therefore, early diagnosis and treatment may be aided by optical coherence tomography’s early identification of small focal abnormalities of the nerve fiber layer.
Epidemiology of Low Tension Glaucoma
Here in the United States
Low-tension glaucoma can affect up to 15–25% of POAG patients. The Baltimore Eye Study found that 33% of those with two measures had an IOP of less than 21 mm Hg, while 50% of people with glaucomatous disc and visual-field abnormalities had an IOP of less than 21 mm Hg on a single visit.
International
In Japan and Korea, low-tension glaucoma is more common.
Mortality/Morbidity
Low-tension glaucoma is associated with loss of peripheral vision.
Race
In Japan and Korea, low-tension glaucoma is more common.
Sex
Females are more likely to get low tension glaucoma.
Age
Patients with low-tension glaucoma are generally older than those with POAG; their average age is 60 years.
History and/or symptoms
Low-tension glaucoma (LTG) may have a history that includes the following:
- Vision loss
- Steroid medication use
- Trauma
- Vasospasm associated with the conditions below:
- Raynaud disease
- Head pain from migraines
- Previous blood loss or a shock-like event might cause coagulopathies.
- systemic hypotension during the night (notably in older thin, white women)
- Immune system diseases (often associated with other autoimmune diseases)
- Vascular systemic disease
- Thyroid disease – Patients with low-tension glaucoma have a higher prevalence of thyroid illness (6 of 25 patients in 1 series)
- Sleep apnea (More so in obese men)
- Alzheimer’s dementia is linked to a slight rise in the cup-to-disc ratio.
- Family history of ocular neuropathy or glaucoma
Differential Diagnosis
The diagnosis of glaucoma requires careful consideration of the patient’s medical history, diurnal IOP fluctuation, optic nerve testing, and visual field assessment. The patient’s history can be used to determine glaucoma caused by steroids and traumatic optic neuropathy. If the optic nerve is cupping steadily, ischemic optic neuropathy (arteritic or nonarteritic) may mimic LTG. Ischemia is also characterized by an immediate onset of visual loss and optic nerve pallor.
Patients with diminished central visual acuity ( 20/40), people under 50, people with visual field deficits that respect the vertical rather than the horizontal midline, and those with optic nerve pallor more severe than cupping may need a thorough workup that includes neuroimaging.
In these circumstances, compressive lesions involving the optic nerve must be ruled out.
The likelihood of neurodegenerative optic neuropathy should be taken into consideration once the more common causes of optic disc cupping have been ruled out. The most aggravating situations are those in which optic disc injury continues even after IOP has been reduced. This category of patients includes a variety of congenital and acquired optic neuropathies, making it difficult for even seasoned observers to distinguish between glaucomatous and nonglaucomatous cupping. Megalopapilla, autosomal dominant optic atrophy, and Leber hereditary optic neuropathy are among the congenital causes of optic disc cupping that can result in an optic disc excavation mimicking glaucomatous optic neuropathy.
The acquired neuropathies may develop as a result of traumatic, toxic, compressive, inflammatory, and/or compressive causes. Although unilateral, a rise in the cup-to-disc ratio caused by optic neuritis might be mistaken for glaucomatous optic neuropathy. Asymmetric optic disc cupping may be caused by compressive lesions such as meningioma, pituitary adenoma, craniopharyngioma, and possibly an internal carotid artery aneurysm and mistakenly ascribed to LTG. Methanol and ethambutol toxicity may result in bilateral optic disc cupping, which is related to axonal degeneration and resembles glaucomatous optic neuropathy. Therefore, more neuro-ophthalmologic research is required when an asymmetrically expanded cup is seen.
Classifying optic disc cupping is now simpler than ever thanks to advancements in diagnostic methods; differentiation between glaucomatous and nonglaucomatous optic disc cupping is made possible by a description of optic disc characteristics combined with imaging of the retinal nerve fiber layer and optic disc topography. Additionally, a thorough review of the patient’s medical history together with an evaluation of the optic nerve’s morphology and functionality aid in the diagnosis of diseases.
Laboratory tests
Depending on the clinical presentation, the following blood tests may be recommended for low-tension glaucoma (LTG):
To rule out anemia, get a CBC count.
Depending on the amount of vision loss, erythrocyte sedimentation rate (ESR) is sometimes measured to rule out anterior ischemic optic neuropathy (AION) in cases with diminished central acuity with a pale nerve.
Request testing for fluorescein treponema antibody (FTA) and rapid plasma reagent (RPR).
To rule out collagen-vascular and autoimmune disorders, antinuclear antibody (ANA) testing is advised. To rule out autoimmune illnesses, testing for extractable nuclear antigens (Ro, La, and Sm) is also advised.
For monoclonal gammopathy, serum immunofixation is recommended. Monoclonal gammopathy (paraproteinemia), which is two-thirds of the time a benign illness, affects 10% of people with low-tension glaucoma. However, if findings from this test are positive, a hemato-oncology expert needs to rule out lymphoproliferative diseases (i.e., malignancies).
Tests for mitochondria in Leber optic neuropathy
Testing for anticardiolipin antibodies (ACA) should be done, and a higher level is thought to be a risk factor for the advancement of visual-field defects.
Imaging
Analyses of the retinal nerve fibers and/or the optic nerve head
Analyzing the retinal nerve fibers and/or the optic nerve head may be useful in identifying the condition and tracking the evolution of glaucomatous optic neuropathy.
Use confocal scanning laser ophthalmoscopy (SLO) or optical coherence tomography to examine the optic nerve head (OCT).
Utilize confocal SLO, OCT, or scanning laser polarimetry to examine the retinal nerve fiber (GDx). Before any abnormalities in visual-field tests, retinal nerve fiber layer abnormalities are frequently possible. Most frequently, the superior and inferior poles experience the initial thinning of the nerve fiber layer.
Compared to CT scanning, MRI of the head and orbits is the recommended imaging modality because of its superior sensitivity in excluding tumors that cause compressive optic neuropathy.
Neuroimaging’s appropriateness for everyday use is up for debate. In case of uncertainty, think about referring to a neuro-ophthalmologist.
Any patient with any of the following conditions should undergo neuroimaging:
- A disease that is clearly asymmetric
- The increased pallor of the optic disc in relation to cupping
- Abnormalities in the visual field, especially those that affect the vertical midline
- The rapid development of visual fields
- The rapid development of ocular neuropathies
- Dyschromatopsia
- Defect in the afferent papillary with a small amount of cupping
- Carotid Doppler examination
To rule out carotid insufficiency, carotid Doppler testing is advised if needed.
Low Tension Glaucoma Causes
The current consensus is that damage to the optic nerve without increased intraocular pressure is caused by either decreased blood flow (perfusion) to the optic nerve (ON) or an optic nerve that is otherwise already vulnerable to damage. While there is still much we don’t know about the causes of low tension glaucoma, this is what we do know.
A family history of low tension glaucoma is regarded as a significant risk factor since this condition can run in families. Age, abnormal blood flow to the optic nerve, diabetes, sleep apnea, Raynaud’s disease, migraines, and structural abnormalities of the tissues surrounding the optic nerve are additional low tension glaucoma risk factors.
Treatment and Studies
A prospective randomized clinical experiment called the Collaborative Normal-Tension Glaucoma Study (CNTGS), which examined the natural course of the condition and the impact of IOP reduction on LTG, produced crucial information. Every eligible subject had one eye randomly assigned to receive either no therapy as a control or a surgical, medicinal, or laser procedure to reduce the IOP by 30% from the starting point. If an eye matched the criteria for a diagnosis of LTG and displayed either proven progression or high-risk field abnormalities that put fixation at risk or the emergence of a fresh disk hemorrhage, it was randomized. In 88% of patients with past recorded progression or field loss threatening fixation, a 30% reduction in IOP prevented visual field progression, as opposed to 65% of the control group.
For certain individuals who have unmistakable advancement in their glaucoma, a combination of surgery and laser treatment is frequently recommended since glaucoma drugs may lower IOP to episcleral venous pressure (range, 8–12 mm Hg). Confirming visual field decline through time and at baseline is crucial. It has been demonstrated that prostaglandin analogues can regulate IOP continuously. B-blockers may speed up the course of LTG in some individuals by causing systemic hypotension and lowering ocular perfusion pressure. B-blocker usage at night may also be avoided due to decreased aqueous humor production and decreased medication effectiveness at night.
The brimonidine 0.2% group in the Low-Pressure Glaucoma Treatment Study (LoGTS) had a lower likelihood of visual field advancement over a 30-month period. However, their IOP reduction was comparable to that of the 0.5% timolol maleate group. This discovery raises the possibility of an IOP-independent neuroprotective mechanism. 9 Additionally, more individuals with medication intolerance left the brimonidine group. As previously mentioned, the systemic hypotensive effects of timolol may also be harmful, which might make it difficult to analyze the study’s findings.
Agents for LTG therapy have not yet been found via neuroprotection research. Memantine, a noncompetitive N-methyl-D-aspartate receptor antagonist, failed to demonstrate effectiveness in phase 3 clinical trials when compared to a placebo. There are a few more mechanisms that are interesting in the hunt for innovative treatments.
Surgery
Because the intraocular pressure (IOP) is already within the standard range, argon laser trabeculoplasty (ALT) may have little impact.
Selective laser trabeculoplasty (SLT): Compared to ALT, SLT causes less tissue damage and scarring while targeting pigment-producing cells in the trabecular meshwork.
Trabeculectomy: For postoperative IOP to be in the single digits following surgery, additional antimetabolite treatment is likely required if medical therapy is inadequate. When aiming for extremely low pressures that may be required to halt or stop the progression of field loss, there is an increased risk of hypotony and endophthalmitis.
Conclusion
Low tension glaucoma is still a difficult condition to manage over the course of a patient’s life. Even though 50% of patients may not advance, those who do could have a serious loss of quality of life and visual field. Clinicians must handle these situations aggressively because IOP lowering is now the sole effective treatment.
FAQ’s
Can blindness be caused by low tension glaucoma?
Normal tension glaucoma and the chance of going blind, Normal tension glaucoma has a 20-year incidence of the blindness of 9.9% in one eye and 1.5% in both eyes.
Which drops work the best for low tension glaucoma?
Latanoprost, bimatoprost, and timolol were shown to be the most efficient IOP-lowering drugs in a comprehensive review and meta-analysis of 15 randomized clinical trials for the treatment of normal-tension glaucoma. The following list of medications is for neuroprotection: Calcium channel blockers
Does low-pressure glaucoma run in families?
Glaucoma predisposition may run in families. However, just because glaucoma runs in your family does not automatically guarantee that you will have the condition. Atypically high intraocular pressure sufferers (IOP). The main risk factor for glaucomatous damage is high IOP.